HISTORY:
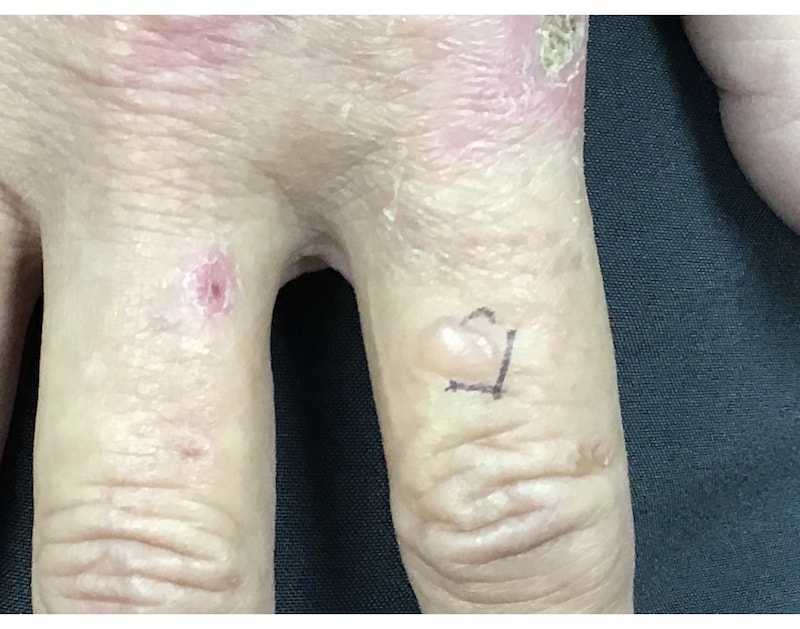
A 50+ year old female presents with a 2-month history of blistering on her hands. This seems to occur with each dose of chemotherapy and then resolves. The patient is receiving treatment (IV carboplatin/paclitaxel) for synchronous primary breast cancer and high grade ovarian cancer and a BRCA1 mutation. The oncologist wondered about herpetic whitlow as the patient has a history of cold sores.
Labs are drawn and a biopsy is taken.
Question: What is the correct diagnosis?
- Epidermolysis Bullosa Simplex (EBS)
- Epidermolysis Bullosa Acquisita (EBA)
- Porphyria Cutanea Tarda (PCT)
- Pseudoporphyria Cutanea Tarda
ANSWER:
3.Porphyria Cutanea Tarda
PATHOLOGY:
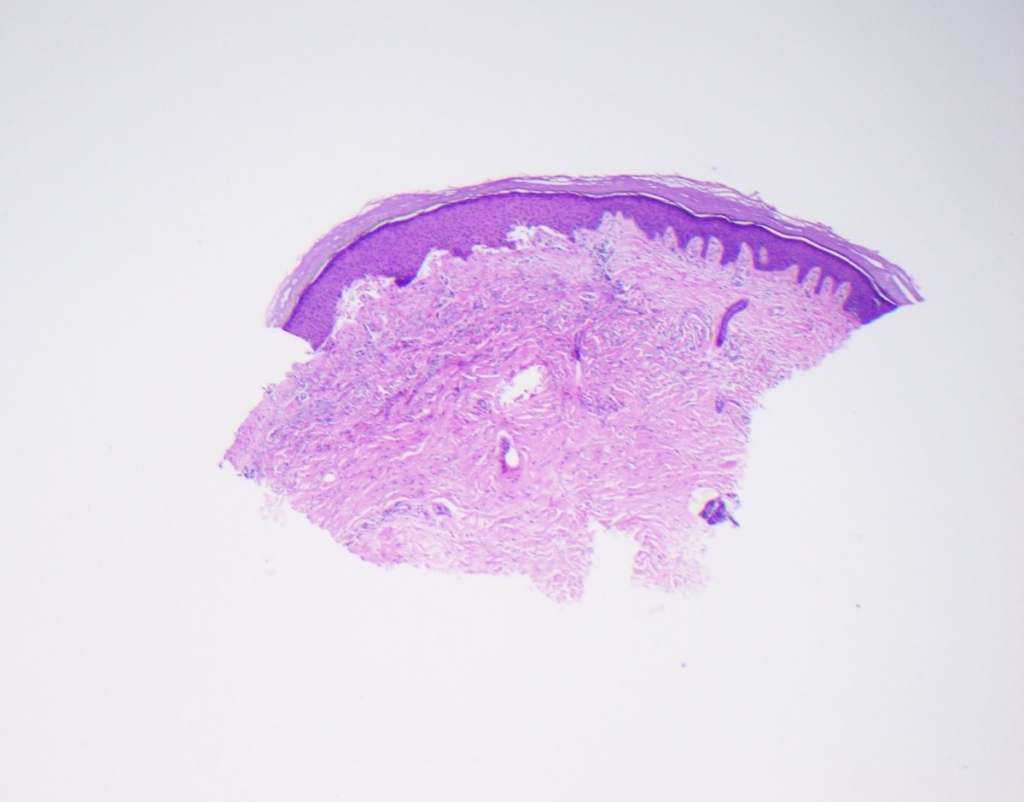
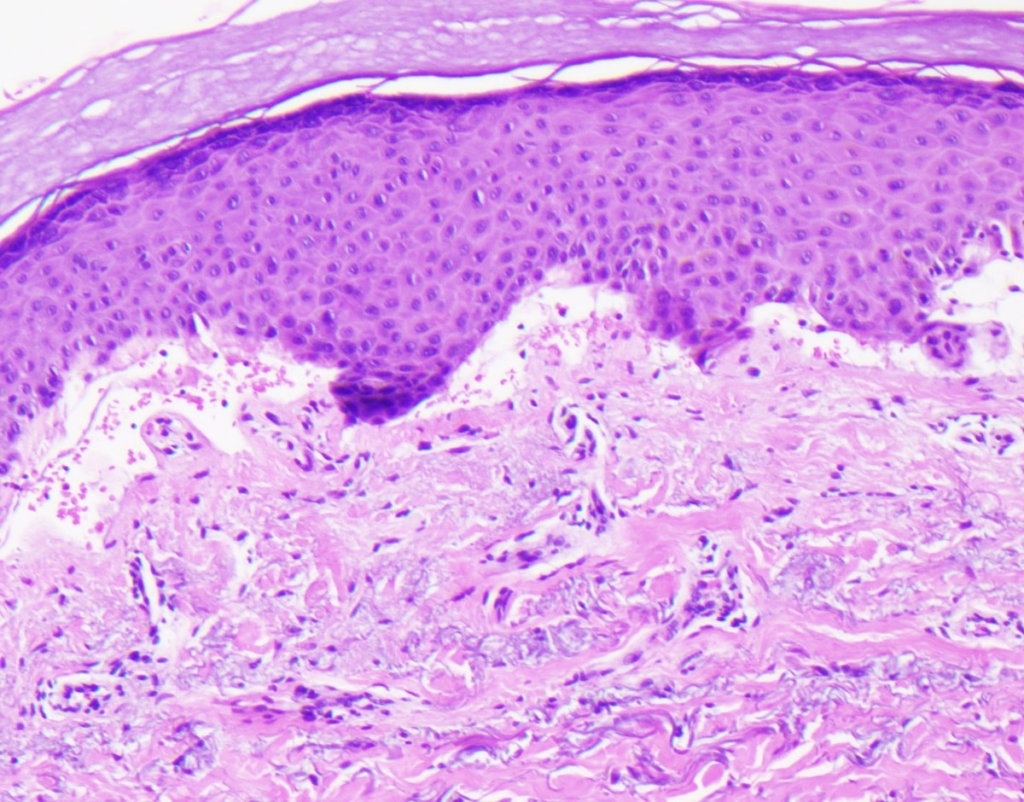
The pathology shows a cell-poor subepidermal blister. Focal caterpillar bodies are seen within the overlying epidermis with some festooning.
SUMMARY:
Labs show plasma with elevated levels of: Urophorphyrin, Hexacarboxyl Porphyrins, and Heptacarboxyl Porphyrins. This is consistent with a diagnosis of Porphyria Cutanea Tarda.
Porphyria Cutanea Tarda (PCT) is the most common of the porphyrias, targeting only the skin. Porphyrias occur with a disruption of the heme synthesis chain of chemical reactions. PCT shows a deficiency of the enzyme uroporphyrinogen decarboxylase (UROD). It is typically an acquired disease, with a genetic component in some patients. Development is usually in mid to late life. Triggers include:
- Liver disease—including alcoholic liver disease
- Alcohol consumption
- Hepatitis B and C
- Iron overload (such as from hemochromatosis, multiple blood transfusions, iron supplementation)
- Estrogens—-including oral contraceptives, hormone replacement therapy, prostate cancer therapy
Pseudo-PCT is caused by renal dialysis or medications (most commonly NSAIDS and diuretics). It shows the clinical features of PCT, but blood and urinalysis do not demonstrate elevated porphyrin levels.
PCT clinically has photosensitivity, appearing on the hands, face and neck. (Usually patients are not aware of the photosensitive trigger.) Skin will show tense vesicles and bullae on a non-inflamed base, skin fragility, hyperpigmentation, hypertrichosis, milia formation, and sclerodermoid changes.
Paclitaxel has been associated with photo-sensitivity and photosensitive rashes. This is the likely trigger for the patient’s PCT given flares with chemotherapy treatments and known association.
FOLLOW-UP:
This patient was managed by her hematologist/oncologist who was also managing her breast and ovarian carcinoma. At diagnosis, she was negative for Hep B and C, HIV, and her baseline ferritin was 616. Her oncologist elected to treat her with phlebotomy, but because of her breast and ovarian cancers and ongoing chemotherapy, a gentle approach to phlebotomy, without regular phlebotomy follow up. The oncologist found that one phlebotomy every few months has kept the patient free of symptoms. She has aimed for a ferritin level of 100, rather than the usual, more stringent 50. The patient was also advised to use sunscreen diligently, and to avoid alcohol.
By: Dr. Robert Korenberg, MD and Dr. Brent Weed, MD