HISTORY:
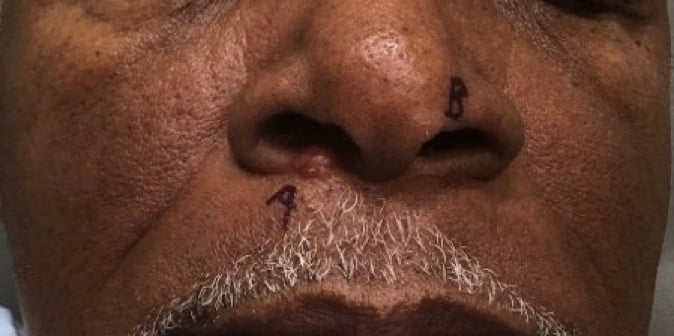
A 60+ year-old man who is a new patient presents with a chief complaint of skin lesions located on the nose. The lesions are irritated, tender pearly telangiectatic papules, present for several years, on the upper cutaneous lip and columella. They are made worse by picking. The patient has no history of skin cancer and has been treating the lesions for two to three years with clobetasol cream received from a prior dermatology office.
Two shave biopsies were performed.
QUESTION: Which blood test should you also consider ordering to identify a suspected “active” disease?
A. CBC
B. Serum amyloid
C. Angiotensin-converting enzyme
D. Vitamin D levels
ANSWER
Best answer is C Angiotensin-converting enzyme
PATHOLOGY
The most well-known serum biomarker in sarcoidosis is serum angiotensin-converting enzyme. It is mainly produced by activated alveolar macrophages and correlates with granuloma burden and radiological stages. This is currently the most frequently used laboratory test in sarcoidosis. Due to the low sensitivity of sACE levels, their value as a diagnostic or prognostic tool remains a matter of debate. Also to keep in mind is that ACE levels in the normal range could in fact be elevated in specific patients. Following ACE levels in a patient may help monitor disease activity and could have a role in predicting treatment outcome. Keep in mind the use of ACE inhibitors in patients with sarcoidosis. If patients with sarcoidosis use ACE inhibitors, serum ACE levels cannot be used in diagnosis or disease monitoring, and should be interpreted carefully.
- CBC – Can detect the two most common disease-relevant hematological findings, namely anemia and leukopenia. Rarely thrombocytopenia can occur. Useful in assessment of dyspnea and to screen for bone marrow involvement
- Serum amyloid – can be increased in sarcoidosis
- Angiotensin-converting enzyme (see above)
- Vitamin D levels – vit D dysregulation is common in sarcoidosis, elevated vit D levels can lead to hypercalcemia and hypercalciuria.
CASE SUMMARY
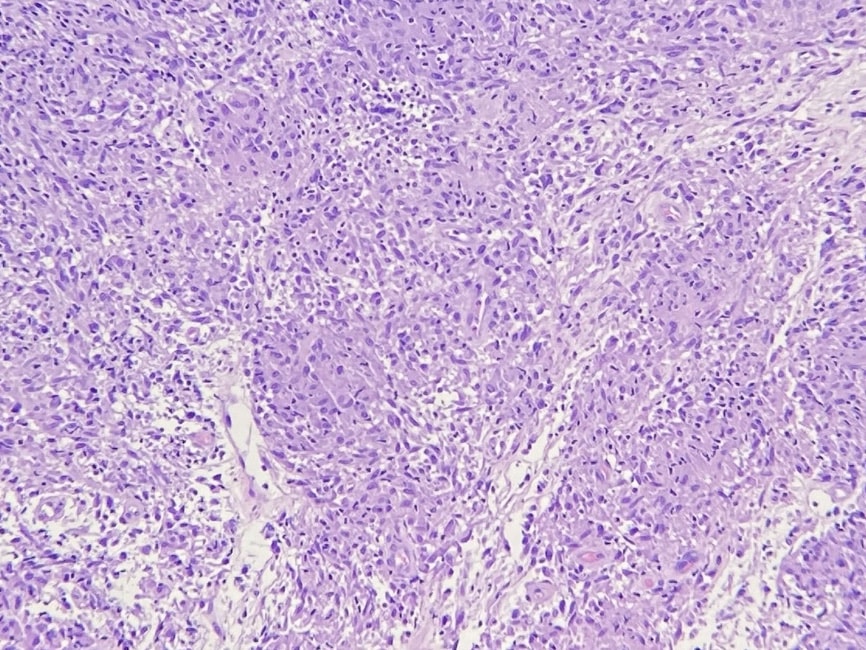
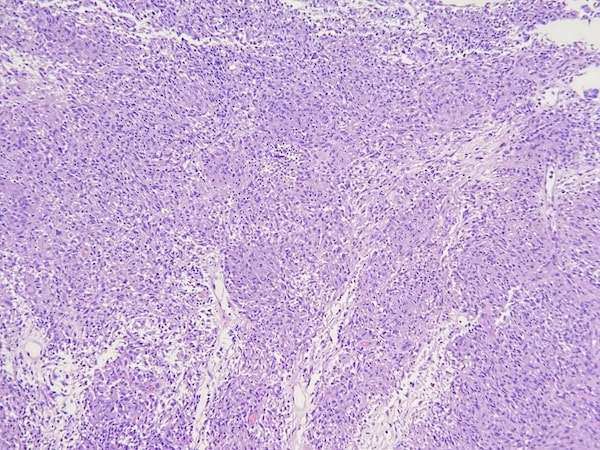
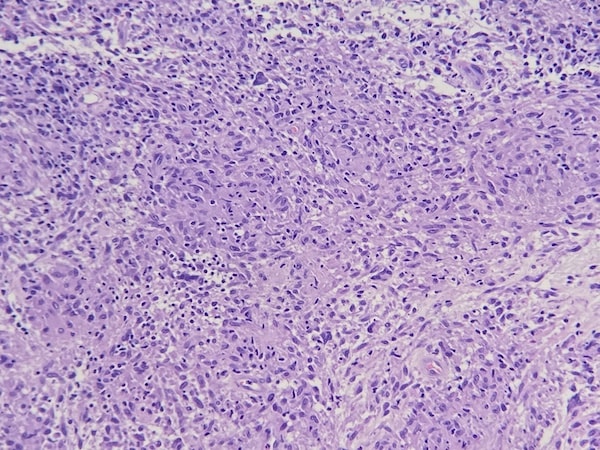
The biopsies show similar features. There is a granulomatous infiltrate of mostly histiocytes with some multinucleated giant cells and some lymphocytes. No polarizable foreign material is present. PAS-D and Fite stains are negative for organisms. These features are consistent with a granulomatous dermatitis, with the differential diagnosis of sarcoidosis or infection. Correlation with clinical photographs and impression favors sarcoidosis.
Sarcoidosis is a multisystem disease characterized by granulomas in various organs including lungs, skin, eye, liver, heart, nervous and musculoskeletal systems. It occurs worldwide. African Americans and Scandinavians have a higher incidence of the disease. Sarcoidosis mainly affects people between 30-50 years of age, and is more prevalent in women, non-smokers, and rural communities. Its incidence is estimated to be between 2.3 and 11 per 100,000 individuals/year and no single cause has been identified. Many researchers have hypothesized the role of genetics, environmental factors, and autoimmunity in the development of sarcoidosis. Cutaneous sarcoidosis can be the presenting sign of systemic sarcoidosis, and work-up is indicated in all patients with cutaneous manifestations.
Lupus pernio is one of the more common forms of cutaneous sarcoidosis. Lupus pernio presents as bluish-red or violaceous nodules and plaques over the nose, cheeks and ears.
A little history: the name is derived from the Latin name for ‘wolf’ (lupus) and for ‘chilblain’ (pernio). It was incorrectly thought to be related to cutaneous tuberculosis, lupus vulgaris.
The prognosis may be worse when there is nasal mucosal involvement and ENT intervention would be indicated. Nasal mucosal involvement can include cartilaginous destruction and nasal collapse leading to saddle nose deformity, and severe rhinitis with crusting and bleeding.
FOLLOW-UP
Chest x-ray and CT scan were recommended to rule out systemic sarcoidosis as nasal involvement is a common indicator of hilar lymphadenopathy. In addition, one may consider obtaining a CBC with diff, CMP and EKG as well as referring to relevant specialists such as cardiology or pulmonology pending results. We may also consider initiating treatment with systemic oral corticosteroids if the patient was unresponsive to topical clobetasol and if there was any systemic involvement.
By: Dr. K. Mireille Chae, MD; Dr. Ashley Dietrich, MD; and Mr. Frank Ferritto, PA-C